News 2018 - Workgroup For The Liver
Main menu:
News 2018
2018/11/07
MANUSCRIPT ACCEPTED: The article entitled "Prospective Assessment of Liver Function by an Enzymatic Liver Function Test to Estimate Short-
In this article, Jara et al. showed that apart from serum creatinine levels, enzymatic liver function measured by LiMAx is an independent predictor of short-
2018/09/10
MANUSCRIPT ACCEPTED: The article entitled "Randomized clinical trial comparing liver resection with and without perioperative assessment of liver function." has been accepted for publication in BJS Open.
In a randomized controlled phase III clinical trial, the impact of perioperative liver function assessment with the LiMAx® test on early postoperative patient outcome and patient management after liver resection had been assessed. The study results demonstrate that the LiMAx® test shortens the length of stay in the ICU and the hospital overall, and it reduces the incidence of severe complications after liver surgery. In contrast to the currently common and cost-
2018/05/03
MANUSCRIPT ACCEPTED: The article entitled "Autofluorescence: A potential pitfall in immunofluorescence-
Abstract: Immunofluorescence (IF) staining of paraffin-
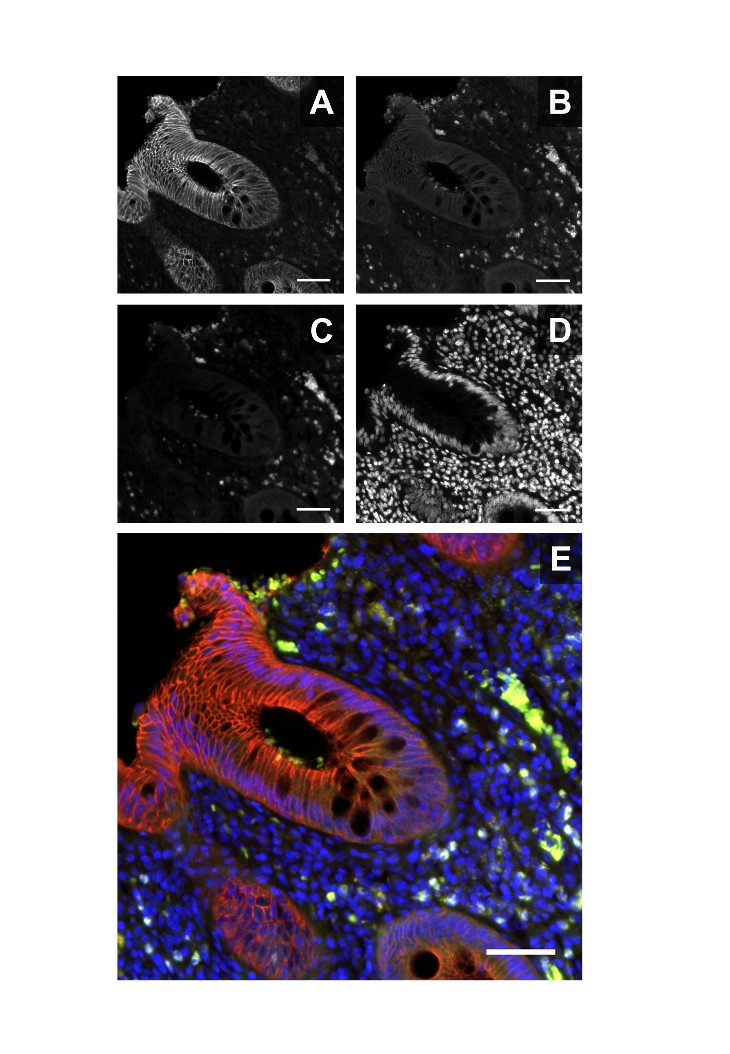
Figure: E-